Diagnostic Labs for Personal Injury and Spine Practices
Diagnostic labs play a critical role in modern medical practices, especially those focused on personal injury, spine care, pain management, and regenerative medicine. While treatment often gets the most attention, accurate diagnostics are what guide clinical decisions, support documentation, and help practices operate efficiently.
For many clinics, diagnostic testing is still handled outside the practice. Patients are referred to imaging centers, specialty labs, or third-party facilities for the studies needed to confirm a diagnosis. While this model works, it can create delays, fragment patient care, and shift significant revenue outside the clinic.
Understanding how diagnostic labs fit into a practice’s workflow and how they can be integrated more strategically can have a meaningful impact on both clinical outcomes and operational performance.
What Diagnostic Labs Actually Do
In a medical practice, diagnostic labs provide the objective data needed to identify and confirm medical conditions. This can include imaging, laboratory testing, or functional diagnostics that help physicians move from symptoms to a clear diagnosis.
For spine, orthopedic, and personal injury practices, diagnostics commonly include:
- X-rays and motion studies
- MRI and CT imaging
- Functional assessments and biomechanical testing
- Blood or laboratory markers used to evaluate inflammation or injury
- Specialized imaging or motion-based diagnostics when standard imaging is inconclusive
Each of these tests serves the same fundamental purpose: providing objective information that helps physicians determine what is actually happening inside the body.
Without accurate diagnostics, treatment decisions rely heavily on symptoms and clinical judgment alone. With reliable diagnostic data, providers can make more informed decisions about care.
Why Diagnostics Matter in Personal Injury Cases
In personal injury medicine, diagnostics play an even larger role than in many other areas of healthcare.
Unlike routine medical visits, personal injury cases often require detailed documentation of the injury itself. Providers must establish not only that a patient is experiencing pain, but also what specific condition is responsible and how it relates to the incident that caused it.
This is where diagnostic testing becomes essential.
Objective findings, whether from imaging, functional testing, or motion analysis, help physicians document injuries clearly and defensibly. In many cases, diagnostic results become a central component of the medical record used by attorneys, insurers, and case reviewers.
When diagnostics are incomplete or inconclusive, cases may remain classified as general “sprain-strain” injuries, which can limit how the injury is understood or documented.

For providers who work regularly in the PI or workers’ compensation space, having access to reliable diagnostics can significantly strengthen both clinical clarity and case documentation.
The Operational Challenge of Outsourced Diagnostics
Despite their importance, diagnostics are frequently handled outside the practice.
A patient visits the clinic, receives an evaluation, and is then referred to an external imaging center or lab for additional testing. The patient must schedule another appointment, travel to a different location, and return later for follow-up.
While this is common, it introduces several operational challenges.
First, it slows down the diagnostic process. Patients may wait days or weeks for imaging appointments and results, delaying treatment decisions.
Second, it introduces friction for patients. Additional appointments and travel can lead to missed studies or incomplete diagnostic workups.
Third, it moves diagnostic revenue outside the clinic. When testing is performed elsewhere, that portion of the care process and its associated revenue remains with the external facility.
For practices that see a high volume of spine or injury cases, this can represent a significant portion of the patient care pathway.
Bringing Diagnostic Capabilities Closer to the Practice
Because of these challenges, some medical practices choose to bring certain diagnostic capabilities closer to their clinical workflow.
This does not necessarily mean replacing major imaging systems like MRI, which often remain centralized in dedicated imaging centers. However, many clinics incorporate complementary diagnostic tools that allow them to evaluate patients more thoroughly without immediately referring them elsewhere.
Examples include:
- In-office digital X-ray systems
- Functional movement and range-of-motion testing
- Ultrasound diagnostics
- Motion-based imaging systems designed to analyze spinal movement
These technologies allow providers to gather meaningful diagnostic information earlier in the patient evaluation process.

Without accurate diagnostics, treatment decisions rely heavily on symptoms and clinical judgment alone. With reliable diagnostic data, providers can make more informed decisions about care.
The Role of Motion-Based Diagnostics in Spine Care
One area where diagnostic technology continues to evolve is the evaluation of spinal motion.
Traditional imaging methods such as MRI and standard X-rays capture static images of the spine. These studies are extremely valuable for identifying structural changes such as disc herniation, fractures, or degenerative conditions.
However, certain spinal issues involve instability or abnormal movement between vertebrae. These conditions may not always appear clearly on static images.
Motion-based diagnostic systems were developed to analyze how vertebrae move relative to one another during controlled movement. By recording spinal motion and measuring alignment, translation, and angulation, providers can obtain objective data about instability that might otherwise be difficult to quantify.
One example of this type of technology is Vertebral Motion Analysis (VMA®), which uses dynamic imaging to evaluate spinal movement and identify ligament instability that may not be visible using static imaging alone.
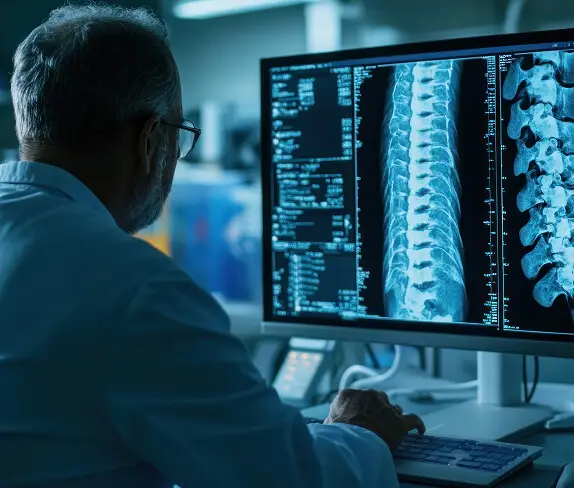
For practices that frequently treat post-traumatic spine injuries, motion-based diagnostics like these can provide an additional layer of clinical insight when traditional imaging does not fully explain a patient’s symptoms.
How Diagnostic Labs Support Practice Growth
Beyond clinical value, diagnostic labs also influence how a medical practice operates.
When diagnostics are integrated into the patient care process effectively, they can help practices:
- Reduce delays in diagnosis and treatment planning
- Improve continuity of care by keeping more services within the practice workflow
- Strengthen documentation for complex injury cases
- Support collaboration with referring providers and legal professionals in injury cases
- Expand the services offered by the clinic
Importantly, the goal is not simply adding technology. The real value comes from integrating diagnostic tools in a way that supports clinical decision-making and improves how the practice functions day to day.

When implemented thoughtfully, diagnostics can become an important part of both patient care and operational strategy.
The Future of Diagnostics in Spine and Injury Medicine
Healthcare continues to move toward more precise, data-driven diagnostics. Providers increasingly rely on measurable, objective findings to guide treatment decisions and support clinical documentation.
Advances in imaging, motion analysis, and functional testing are helping physicians better understand injuries that were previously difficult to quantify.
For spine and personal injury practices, this shift means diagnostics will likely continue playing a larger role in both patient evaluation and practice operations. Clinics that understand how to integrate diagnostic capabilities effectively are often better positioned to provide comprehensive care and deliver better outcomes for their patients.
